Professor Sir Malcolm Grant OBE
Ed Smith, CBE, FCA
Ciaran Devane
Margaret Casely-Hayford
Dame Moira Gibb
Lord Victor Adebowale
Professor Sir John Burn
Noel Gordon
David Roberts
Simon Stevens
Professor Sir Bruce Keogh
Jane Cummings
Dame Barbara Hakin
Paul Baumann
Tim Kelsey
Karen Wheeler
Ian Dodge
25 March 2015
Dear Board & Executives of NHS England,
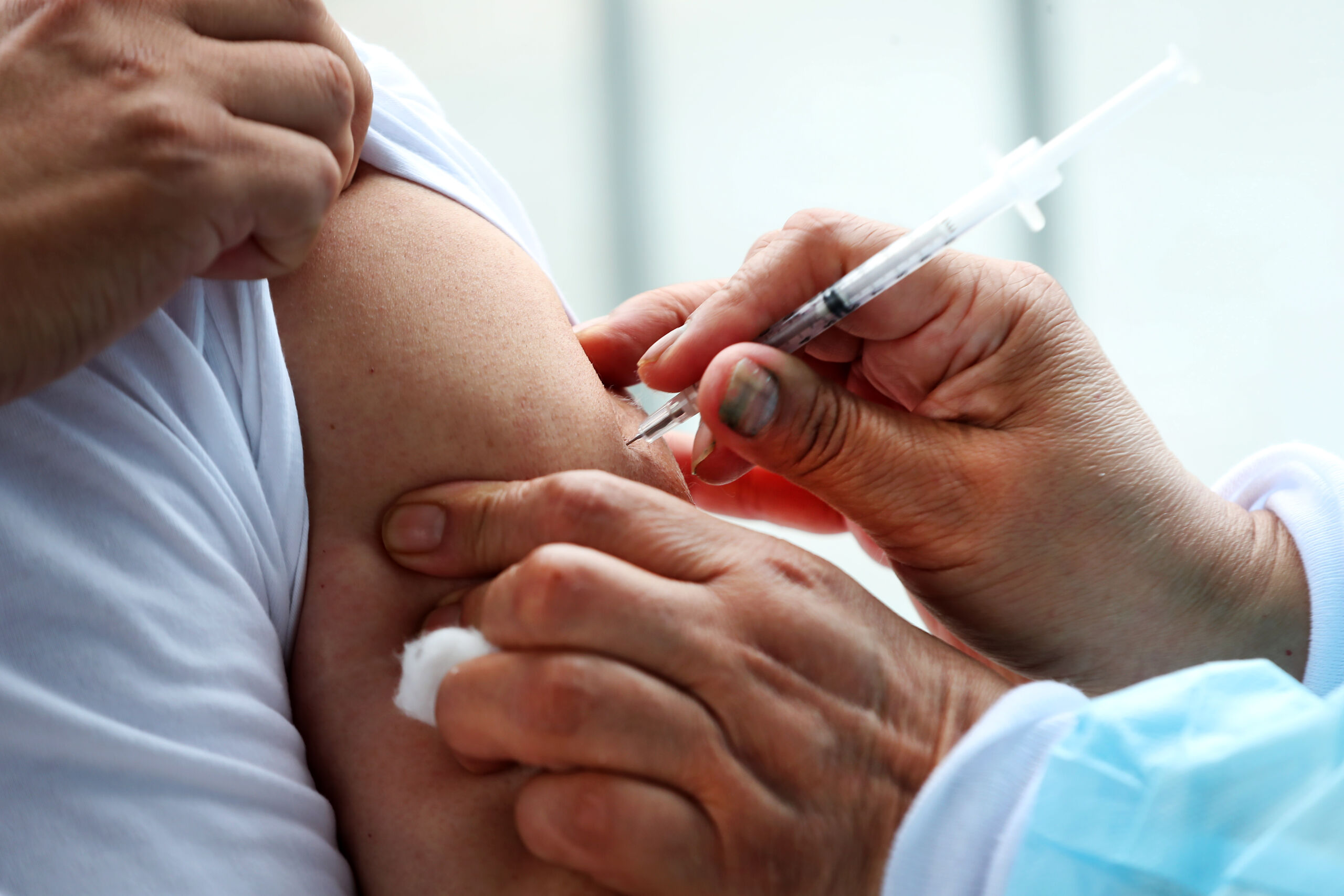
TSC Patients facing avoidable harm and risk of death
We are writing to you on a matter of extreme urgency. As you will know, prescribing policies for Everolimus to treat brain tumours (SEGA) and kidney tumours (AML) in patients with Tuberous Sclerosis Complex (TSC) have been under development for some time. Although we are aware that these policies are “under consideration for prioritization” for NHSE’s 2015/16 work-programme, no timelines for decision-making have been revealed. In the event that the policies are prioritized there has been no indication for the time-line to a decision being reached and we have therefore concluded that the best-case scenario is for a prescribing policy to be in place for the financial year 2016/17.
In the meantime, and since a policy is under development, IFR pre-screening panels are turning away individual funding requests with no right of appeal. In the event that an application does make it to panel the overwhelming likelihood is that it will be turned down on the grounds that the patient cannot be proved “exceptional”. As you will be aware, in the case where there are more than 5 patients seeking funding for a licensed product that has such a high likelihood of improving the patient’s condition, then proving exceptionality is a near impossibility. Furthermore, it is nonsense to apply this criterion in the case of an effective, licensed product for whom such a cohort exists.
The current position is this; around 32 patients with critical need, whose doctors believe Everolimus treatment is their best or only option, have no hope of access to funding. Most have been waiting many months. Approximately half of these patients are at imminent risk of a catastrophic event (renal bleed or kidney failure) with a high risk of preventable death.
All official correspondence so far received on this matter that by the TSA, by MPs acting on behalf of their constituents and by patients and their families, has cited IFRs as a viable route to funding. This is demonstrably not the case.
It has been made clear by officials that ministers cannot intervene and that the power to introduce an interim funding policy to avoid needless suffering and death lies with NHS England. With power resides the responsibility and we urge you to act upon it.
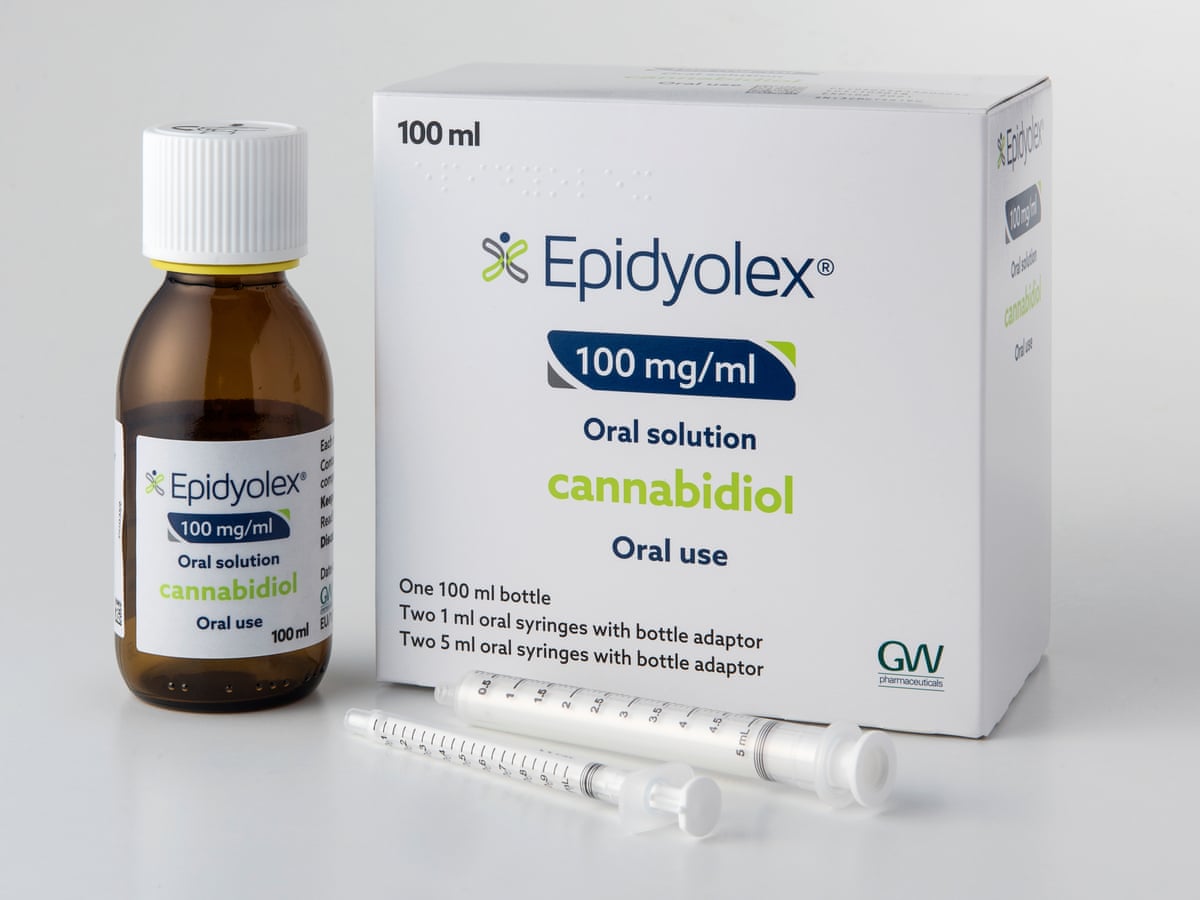
Everolimus is a highly effective drug treatment, recommended by international guidelines, widely reimbursed outside England, the cost of which approximates to the average cost of treating renal failure and dialysis (c£36K pa). Whilst we entirely accept that there needs to be a process of evaluation, the delays in NHS England’s work programme have resulted, and will further result in, avoidable harm. This issue affects real people. They are mothers and fathers with small children. They are young adults struggling to be well enough to access education and employment. They are young children who deserve access to the healthcare they need. They cannot afford to sit it out whilst NHS-England resolves its current issues.
We understand perfectly that NHS England would not wish to be funding “access for life” to Everolimus for patients granted access on an interim basis. However, this argument does not hold water in the case of TSC and Everolimus when you consider that the estimated cost per patient per year on hospital haemodialysis (£35,000) is comparable to the cost of Everolimus (£36,000). No patient should be facing death, no parent should be facing the death of a child, for the sake of process inertia, or for fear of adding £1,000 per year to his or her NHS bill should they survive. We urge you to inject a sense of reality and urgency to this situation and provide for access for those in critical need.
Sincerely,
Professor Pamela Crawford, MBChB FRCP
Consultant Neurologist
Dr Hannah Cock, BSc MD FRCP
Reader & Honorary Consultant Neurologist
Dr Frances Elmslie MD FRCP,
Consultant Clinical Geneticist
Dr Rosemary Ekong, PHD
Senior Research Scientist
Dr Eric Finlay, MBChB MSc FRCPCH MRCP DCH
Consultant Paediatric Nephrologist
Dr Alan Fryer, BSc, MB BS MD FRCP FRCPCH
Consultant Clinical Geneticists
Dr Daniel Gale, MA MB BChir MRCP PhD
Clinician scientist and honorary consultant nephrologist
Simon Johnson BSc MBBS DM FRCP
Professor of Respiratory Medicine
Dr Sheilagh Joss, MBChB, MRCPCH, Med
Consultant Clinical Geneticist
Dr Chris Kingswood, MRCS, MRCP, FRCP
Consultant Neprhologist, Brighton and Sussex University Hospital
Dr. Graham Lipkin, MB ChB, BSc, MD, FRCP
Nephrology – Consultant
Prof Patrick J Morrison, CBE MD DSc FRCP FRCPI FRCPCH FFPHMI Consultant in Genetic Medicine, Belfast Health and Social Care Trust
Uday Patel, MB. CLB MRCP FRLR
Consultant Radiologist, St Georges
Professor Emeritus Sue Povey, MD
Dept of Genetics, Evolution and Environment, UCL
Dr F Lucy Raymond MA DPhil FRCP
Reader in Neurogenetics & Honorary Consultant in Medical Genetics
Professor Julian Sampson DM, FRCP, FMedSci
Co-Director, Institute of Cardiff Cancer & Genetics
Dr Charles Shepherd,
Consultant Paediatrician
Dr. Andrew Robert Tee, Ph.D., B.Sc.
Senior Lecturer
Dr Neil PJ Walker, FRCP
Consultant Dermatologist
Jayne Spink
On behalf of the Tuberous Sclerosis Association
To whom correspondence should be sent for distribution to signatories:
Jayne Spink, Tuberous Sclerosis Association
jayne.spink@tuberous-sclerosis.org